You might assume your inhaler works because it isn't expired, but temperature and humidity often ruin it long before the date on the box. According to recent studies, up to 12% of asthma treatment failures during emergencies happen simply because the device wasn't stored correctly. When you're gasping for air, you don't want to find out your albuterol stopped working because it sat in your hot car. Today, we are breaking down exactly how to protect your life-saving medication so it works when you need it most.
Why Storage Conditions Change Medicine
The chemicals inside your inhaler aren't static; they react to their environment. Manufacturers spend millions testing stability protocols to ensure the dose you breathe in matches the label. However, once you leave the pharmacy, that control ends. Exposure to temperatures above 86°F (30°C) can cause the propellant in metered-dose inhalers to lose pressure. In extreme heat, like a parked car reaching 158°F in summer, the medication can denature completely within 30 minutes.
This isn't just about comfort; it's about molecular integrity. For example, dry powder formulations rely on specific crystal structures to disperse into your lungs. If the relative humidity exceeds 60%, the powder clumps together. You press the button, nothing comes out, and you think the medicine ran out early. Research from the University of North Carolina shows that improper storage reduces drug delivery efficiency by as much as 40%. That means a single puff provides less than half the relief intended.
Different Devices Need Different Care
Not all devices store the same way. Treating a nebulizer solution like a metered-dose inhaler could lead to contamination, while storing a dry powder device in a humid bathroom destroys its mechanism. Here is what you need to know based on your specific equipment:
| Device Type | Ideal Temperature | Humidity Limit | Critical Risk |
|---|---|---|---|
| Metered-Dose Inhaler (MDI) | 59°F to 86°F (15°C-30°C) | <60% | Loss of propellant pressure |
| Dry Powder Inhaler (DPI) | 68°F to 77°F (20°C-25°C) | <50% | Clumping of powder capsules |
| Nebulizer Solution | 36°F to 46°F (Fridge) / Room Temp | Sealed until use | Bacterial growth once opened |
For standard pressurized cans like ProAir HFA, keeping them below 86°F is the golden rule. You never want to puncture them or throw them in fire, as they are pressurized containers. On the other hand, nebulizer solutions are trickier. Many liquid ampules like Pulmicort require refrigeration initially to stay sterile. Once you open a multi-dose vial, it usually has a shelf-life of only 7 days at room temperature. Keeping track of when you first opened the bottle is just as important as the expiry date stamped on the factory label.
The Hidden Dangers in Your Home
We often place our meds where they are most convenient, but convenience is rarely safe for pharmaceutical stability. The kitchen and bathroom are the two biggest offenders in a household survey by the Johns Hopkins study. The kitchen sees rapid temperature swings from ovens and dishwashers, creating micro-climates that fluctuate beyond the "room temperature" range. Meanwhile, bathrooms are notorious for spikes in humidity after a shower, which destroys moisture-sensitive capsules in devices like Spiriva HandiHaler.
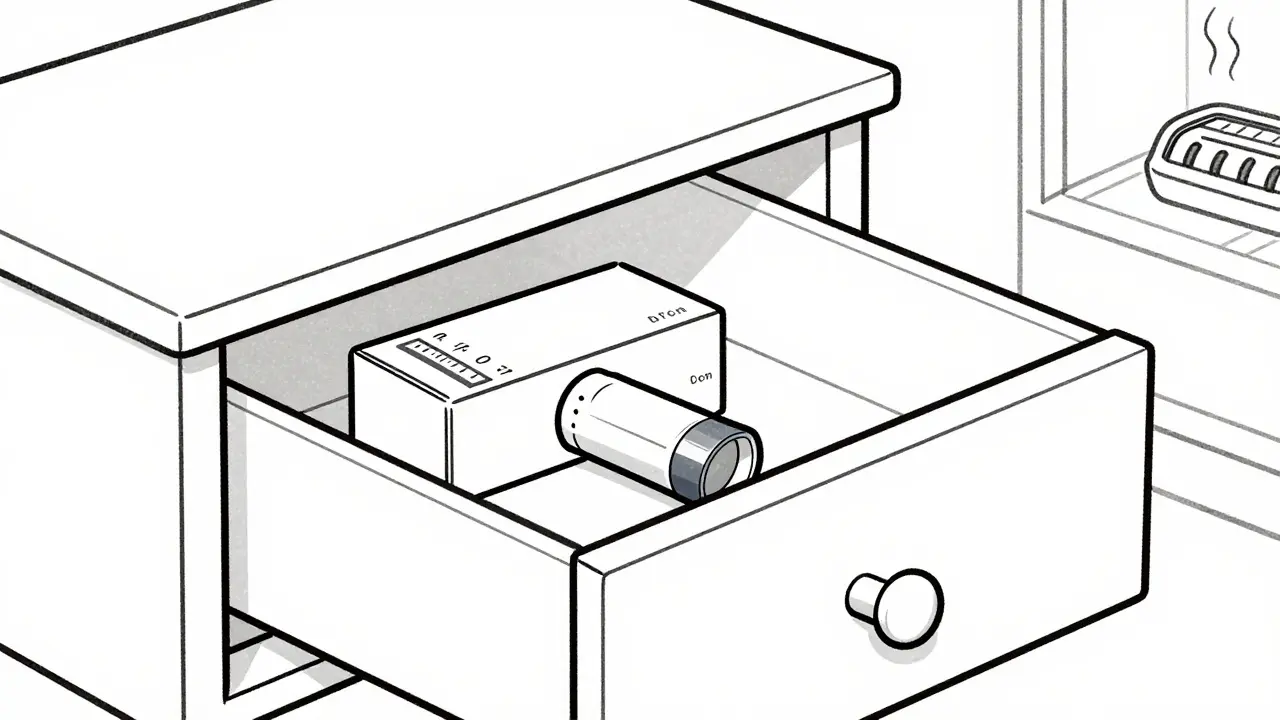
To combat this, you need a dedicated "medication corner." A bedroom dresser drawer away from windows works well. It stays cool, dark, and dry. If you live in a region with high year-round humidity, consider using a small digital hygrometer to monitor the air quality in that spot. Ideally, you want the storage area maintained between 40-50% humidity. This simple step prevents the invisible damage that ruins the powder texture inside your DPI.
Traveling With Rescue Medication
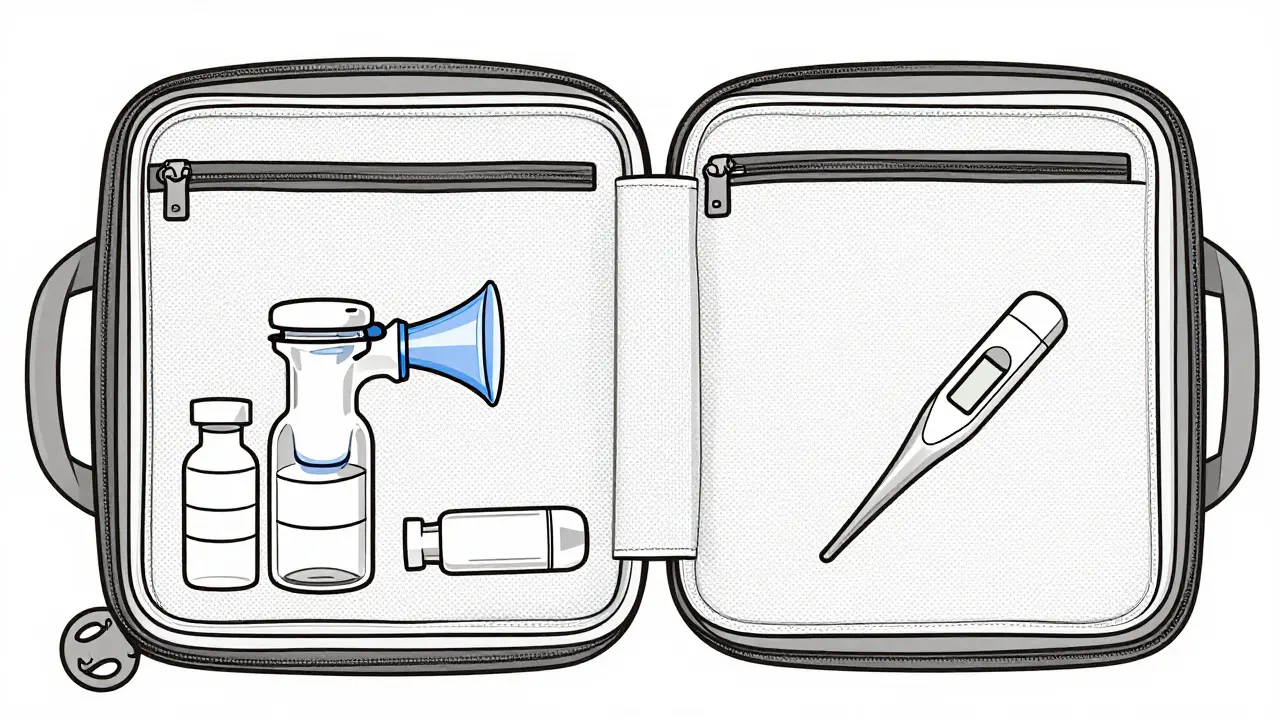
Leaving home adds another layer of complexity. Summer travel is particularly risky for patients who keep their inhalers in the car. Even in short stops, a vehicle interior acts like an oven. Experts recommend the "Rule of 15": do not let your medication sit outside controlled temperatures for more than 15 minutes. For longer trips, insulated hard cases designed for medication, such as the MediSafe bag, provide essential thermal regulation.
When flying, security checks can force you to remove items, increasing exposure time. Always carry your medications in your carry-on luggage, never checked bags. The hold of an airplane can reach freezing temperatures or spike in heat if cargo loading isn't climate-controlled. Additionally, keep a backup dose in a separate piece of luggage so a total loss doesn't leave you without a rescue plan. By 2026, many smart cases now feature Bluetooth sensors that alert your phone if the internal temp drifts, adding a layer of peace of mind during vacations.
Safety First: Disposing of Old Units
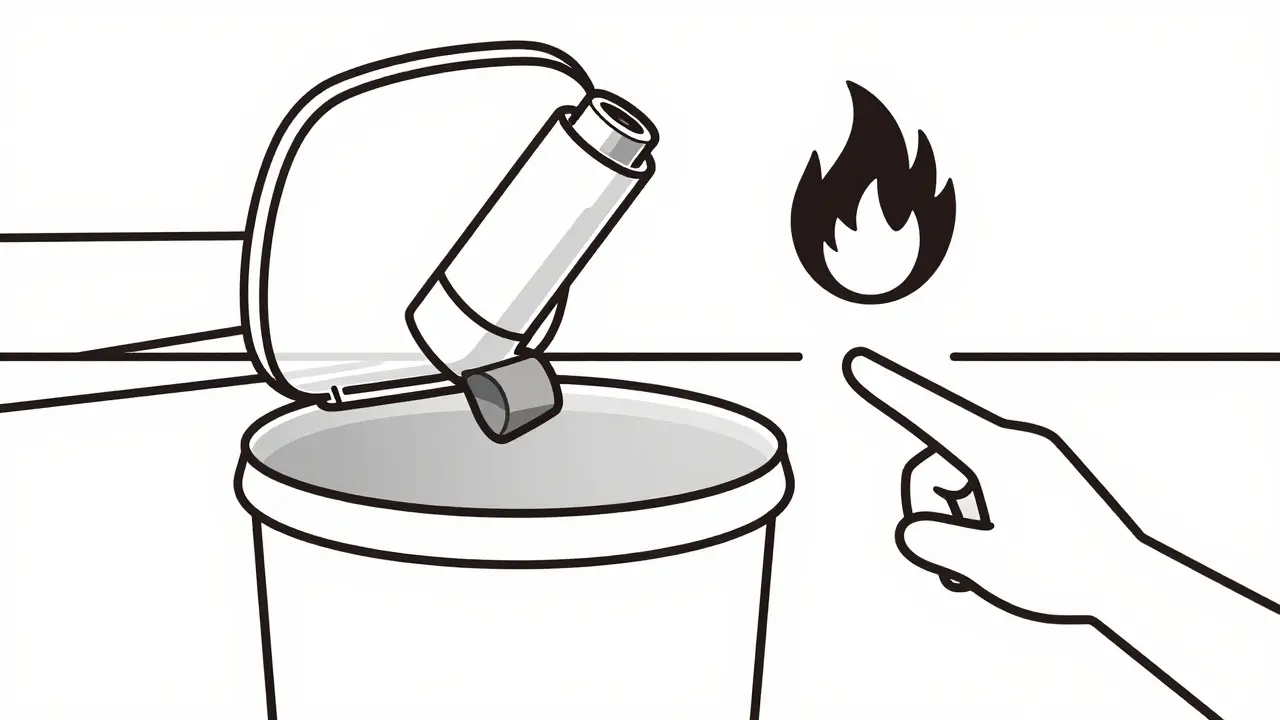
Once your inhaler is empty or expired, handling it requires care. Never puncture the canister to speed up disposal, as this can release flammable propellants or cause injury. Most manufacturers advise against incineration due to the explosion risk. Instead, place the used metal canister in your regular trash bin unless your local pharmacy offers a specific take-back program. For nebulizer cups, clean them thoroughly with warm soapy water every day. Let them air dry on a clean towel; placing wet parts in a closed container promotes mold growth.
If you have unopened bottles of nebulizer solution that have passed their expiration, bring them to a designated collection site. These contain active pharmaceutical ingredients that shouldn't enter the sewage system. Improper disposal contributes to environmental contamination, and in some regions, flushing is illegal. Always check local waste management guidelines for the correct protocol for hazardous liquid waste.
Troubleshooting Common Failures
Even with the best intentions, mistakes happen. If you notice the mist feels weak or tastes different, stop using the device immediately. Check the counter window on the bottom of your inhaler. If it shows zero doses left, replace it even if the physical canister still contains some fluid. The residual liquid lacks the correct concentration. For travel-related doubts, if you've been in extreme heat for more than a few hours, consult your pharmacist. They may advise replacing the unit rather than risking a failure during an attack.
Keep a log of when you buy new prescriptions. Mark the purchase date directly on the device box with a marker. This creates a clear visual reminder that the 1-year expiration starts then, not when you run out. Digital reminders via health apps can also ping you to check your storage conditions before heading out on summer days.
Frequently Asked Questions
Can I store my inhaler in the bathroom cabinet?
It is generally not recommended. Bathrooms experience frequent fluctuations in heat and humidity from showers, which can degrade the medication inside, especially dry powder inhalers.
Does cold weather hurt my inhaler effectiveness?
Extreme cold can thicken the suspension inside the canister, making it spray poorly. Bring the inhaler into a warm indoor environment for at least 15 minutes before using it.
How do I know if my nebulizer solution is bad?
Check for cloudiness, discoloration, or particles floating in the liquid. If the solution looks anything other than clear, discard it immediately.
Should I keep my inhaler in my car glove box?
No. Car interiors can exceed 150°F (65°C) in summer, destroying the chemical structure of the medication. Keep it in your pocket or an insulated case instead.
Do I need to keep my inhaler in the original box?
Yes. The cardboard box blocks light and protects the plastic from physical damage. It also holds the instruction leaflet which lists critical storage limits.


Comments
15 Comments
Monique Ball
You really have to pay attention to the details about temperature control.
Most people just toss the inhaler in the glovebox without thinking twice.
That is exactly how the propellant loses its pressure integrity over time.
I have seen friends struggle because their device failed during an attack.
It is absolutely tragic when prevention was possible all along.
The molecular structure breaks down when heat spikes above thirty degrees celsius.
Humidity makes dry powder clump into useless chunks inside the capsule.
We often forget that bathrooms are terrible places for medicine storage.
Steam from a hot shower ruins the stability of those fragile particles instantly.
A simple bedroom drawer works infinitely better than a bathroom cabinet.
Traveling requires even more strict adherence to the fifteen minute rule.
Leaving meds in a parked car is asking for total degradation.
Smart cases help monitor the internal environment effectively now.
Disposal methods also matter for safety reasons regarding pressurized cans.
Everyone needs to understand that expiration dates aren't the only metric that counts.
Thank you for putting together such a comprehensive resource for us.
Aaron Olney
the heat stuff is scarry 😱
i left mine in teh car last summer and it felt weak when i used it
didnt know why until now
thanks for the info guys!!
would have been dead otherwise lol 🤣
Philip Wynkoop
Bathroom storage is definitely the biggest mistake people make with these devices.
Jeannette Kwiatkowski Kwiatkowski
It is fundamentally important to realize that convenience is the enemy of efficacy.
The average person lacks the scientific literacy required to maintain pharmaceutical integrity.
We see this ignorance everywhere in public health discussions.
Proper storage protocols are not optional suggestions but absolute requirements.
One does not want to rely on chance during a respiratory crisis situation.
This guide articulates the nuance that most manufacturers gloss over completely.
Temperature fluctuations are silent killers of therapeutic value.
Paul Vanderheiden
totally agree with you
sometimes we just want easy access but safety comes first for sure
hope everyone checks their drawer setup soon
we can all learn a lot from this thread today
keep your breathing safe always
Sabrina Herciu
It is critical to note the difference between MDIs and DPIs regarding humidity thresholds.
Many patients conflate the two mechanisms despite distinct storage needs.
Propellants react differently to thermal expansion compared to crystal powders.
Maintaining a log helps track when vials were opened versus factory expiration.
Pharmacists often emphasize shelf life but neglect environmental factors.
Patient education materials frequently omit specific humidity percentages.
This oversight contributes significantly to non-adherence issues clinically.
Rohan Kumar
they just want us to buy new boxes constantly 🙄
storage guidelines sound scary for profits
pharma companies love when meds go bad fast
conspiracy theory alert ☂️
trust me on this one haha 😂
Jordan Marx
The underlying mechanism involves propellant thermodynamics and crystal lattice stability parameters.
Relative humidity acts as a solvent for hygroscopic compounds within the formulation.
Thermal excursions above the glass transition temperature degrade polymer casings too.
Bioavailability drops precipitously when physical form factors collapse internally.
Patients should utilize calibrated hygrometers to monitor micro-environments accurately.
Sarah Klingenberg
Its nice to see such clear info posted here :)
People often forget how sensitive medicine can be to our daily habits.
Just keep things cool and dry and you should be fine most of the time.
Happy holidays to everyone reading this thread!
kendra 0712
So glad someone wrote this up!!!
We really need to take care of our health equipment properly!
Summer trips can be so tricky with temperature control rules.
I am going to buy a smart case next week for sure!
Knowledge is power when staying healthy!
Sophie Hallam
The distinction between device types is a vital point for safety.
Humidity levels in bathrooms fluctuate far beyond safe limits for powder inhalers.
Bedroom drawers offer a more stable environment for consistent dosing.
Tracking open dates is a practical habit for managing inventory effectively.
Safety protocols should always prioritize patient outcomes over convenience.
Richard Kubíček
Perhaps the true danger lies in our assumption of permanence regarding chemical substances.
We trust labels implicitly while ignoring the entropy of our environment.
Responsibility rests heavily on the individual to safeguard their own well-being.
Nature demands order that we must enforce through deliberate action.
gina macabuhay
Carelessness with medication storage is morally indefensible given the stakes involved.Strict adherence to storage protocols should be mandatory for all patients.
You cannot claim ignorance when clear guidelines exist publicly.
No excuses apply when lives depend on proper maintenance procedures.
Monique Louise Hill
That is a harsh view but it is the truth 💯
We must police ourselves better on these hygiene basics.
Ignoring advice puts everyone in the community at risk eventually.
Stay responsible please! 👇
Austin Oguche
In many regions where humidity is high year round these precautions are essential.
Different climates require different approaches to pharmaceutical preservation.
Global standards vary but the science remains consistent across borders.
Sharing this knowledge aids cultural understanding of health management practices.
Write a comment