The reality is that generics now make up about 90% of all prescriptions dispensed in the US. This massive shift isn't just about cost-cutting; it's backed by a regulatory framework that ensures a generic isn't just a "cheaper version," but a therapeutic twin. If you're still weighing whether to push for a generic switch in a high-stakes case, the data suggests that for the vast majority of drug classes, the outcome is identical.
The Science of Bioequivalence
Before a generic hits the pharmacy shelf, it has to pass through a rigorous gauntlet. The core of this is Bioequivalence is the demonstration that a generic drug delivers the same amount of active ingredient into the bloodstream at the same rate as the brand-name drug . This is managed under the Abbreviated New Drug Application (or ANDA), a pathway created by the 1984 Hatch-Waxman Act to bypass the need for repeating massive clinical trials if the drug is chemically identical.
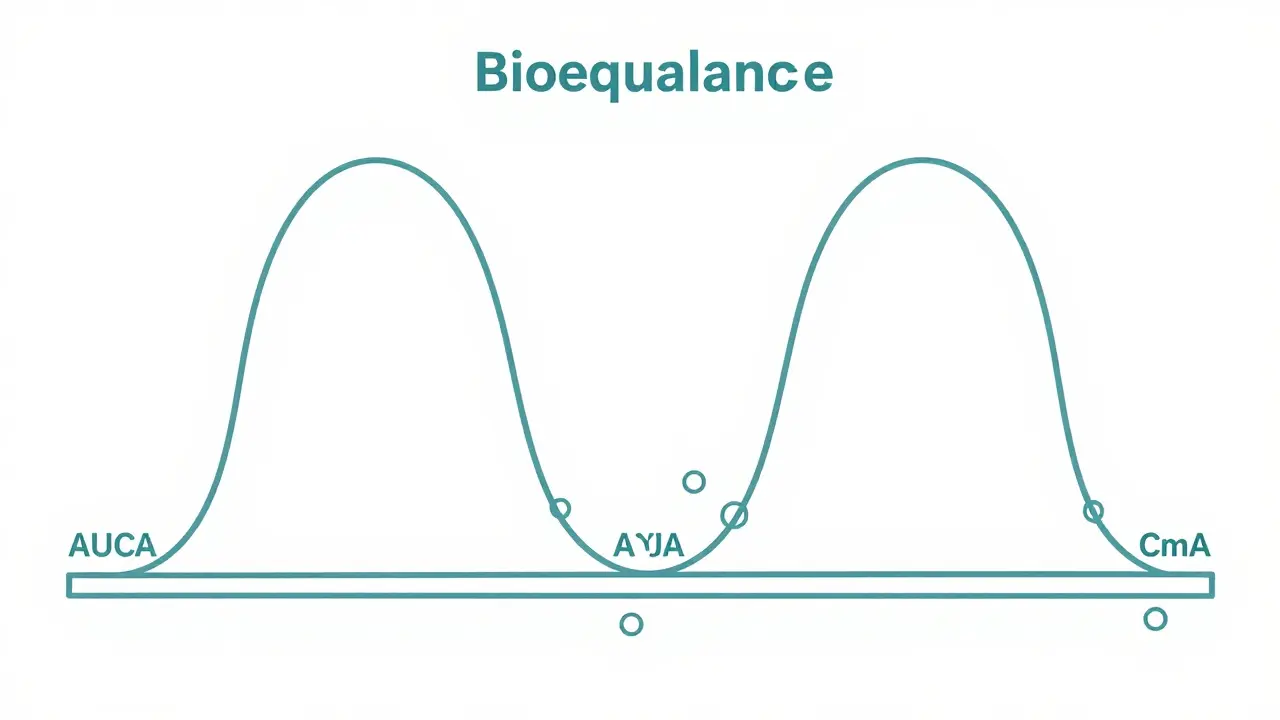
To get approved, a generic must fall within a strict 80-125% range of the pharmacokinetic parameters of the reference drug. This means the AUC (Area Under the Curve), which measures total drug exposure, and the Cmax (peak concentration) must be nearly identical. For most drugs, this is a straightforward process. However, for Narrow Therapeutic Index (NTI) drugs-where a tiny change in dose can lead to toxicity or treatment failure-the standards are even tighter. For example, a 2020 study in Nature Scientific Reports looked at transplant recipients using tacrolimus and found no clinical difference when switching between brand and generic versions over 42 days.
What the Big Studies Actually Show
If you look at the population-level data, the results are overwhelmingly in favor of generics. A massive study published in PLOS Medicine used propensity score matching across 14 different clinical endpoints. Out of 16 comparisons, 12 showed absolutely no statistically significant difference (p>0.05) between generic and brand users. In some cases, generics actually looked better. For instance, patients using generic amlodipine showed slightly superior cardiovascular outcomes compared to those on the brand name.
| Drug Class / Medication | Clinical Outcome Measured | Finding (Hazard Ratio) | Result |
|---|---|---|---|
| Cardiovascular (Quinapril) | Hospitalization for MI or Stroke | 0.99 [0.94-1.05] | Equivalent |
| Bone Health (Alendronate) | Non-vertebral Fracture Rates | 1.00 [0.96-1.05] | Equivalent |
| Diabetes (Glipizide) | Insulin Initiation Rates | 1.01 [0.97-1.05] | Equivalent |
| Psychiatric (Sertraline) | Psychiatric Hospitalization | 1.07 [1.01-1.14] | Slightly Higher Risk |
It's worth noting the psychiatric medications. The data showed a slightly higher rate of hospitalization for generic users of sertraline and escitalopram. But here is the catch: when researchers looked at "authorized generics" (the brand-name drug sold without the brand label), they saw the same pattern. This suggests the issue isn't the generic formulation itself, but perhaps the types of patients who are shifted to generics-often those with less social support or different insurance coverage.
Navigating the "Orange Book" and Ratings
For a provider, the most practical tool for decision-making is the Orange Book, which is the FDA's official publication listing all approved drug products with therapeutic equivalence evaluations . When you look up a drug, you'll see it's either "A-rated" or "B-rated."
- A-Rated: These are therapeutically equivalent. They have the same active ingredient, dosage form, and strength, and are expected to have the same clinical effect. About 97% of generics fall into this category.
- B-Rated: These are not considered therapeutically equivalent. This doesn't mean they are useless, but they might have a different release profile or a different inactive ingredient that could matter for some patients.
If you see a B-rating, that's when you should exercise caution. This is especially true for complex delivery systems like inhalers or topical creams, where the way the drug is delivered is just as important as the chemical itself. The FDA's 2022 guidance on complex generics emphasizes that these products require more specialized bioequivalence testing because a simple blood test (AUC/Cmax) doesn't tell the whole story of how an inhaler performs in the lungs.
Patient Perception vs. Clinical Reality
We've all had the patient who swears the generic "doesn't work" but the brand-name one does. This is often a psychological response to the physical appearance of the pill. Inactive ingredients-the fillers, dyes, and binders-can change the color, shape, or taste of a tablet, even if the active drug is identical. A 2019 FDA study confirmed that these physical differences have zero impact on clinical outcomes.
Interestingly, real-world data from 3.5 million Medicare beneficiaries showed that generic users actually had higher five-year survival rates (85.9%) than brand-name users (77.8%). Now, that doesn't mean generics make you live longer. When researchers adjusted for health factors (using inverse probability of treatment weighting), the gap narrowed. It turns out that healthier patients are more likely to be prescribed generics, while the sickest patients are often kept on brand names by their doctors. The "advantage" was a result of the patient's starting health, not the drug's performance.

Practical Tips for Providers
When discussing generics with a skeptical patient, avoid saying "it's the same thing." Instead, explain the 80-125% bioequivalence rule. Tell them that the FDA mandates that the drug must hit the bloodstream at virtually the same speed and concentration as the original. This moves the conversation from an opinion to a regulatory standard.
For the vast majority of cardiovascular, metabolic, and CNS drugs, the evidence is clear: the risk of an adverse outcome from switching to an A-rated generic is negligible. In fact, the FDA's Adverse Event Reporting System showed that only 0.02% of adverse reports were generic-specific, while 3.2% involved brand-name drugs. The safety profile is not just equal; in terms of reported incidents, it's often cleaner.
Do generic drugs have the same side effects as brand-name drugs?
Yes, because the active ingredient is identical, the primary side effect profile is the same. However, some patients may react differently to the inactive ingredients (fillers or dyes), which can vary between manufacturers. This is rare but is the primary reason some patients may feel a difference.
Are there any drug classes where I should avoid generics?
Generally, you should be more cautious with Narrow Therapeutic Index (NTI) drugs or complex generics like certain inhalers. Always check the FDA Orange Book; if a drug is "B-rated," it is not considered therapeutically equivalent and may require closer monitoring during a switch.
What is the difference between a traditional generic and an authorized generic?
An authorized generic is the exact same product as the brand-name drug, manufactured by the original company but sold without the brand name. Clinical data shows they are therapeutically identical to both the brand and traditional generics, though some patients accept them more easily because they are the "original" formula.
How long does the FDA take to approve a generic drug?
On average, the review time for an Abbreviated New Drug Application (ANDA) was about 10 months in 2022. This process ensures the manufacturer meets all bioequivalence and quality standards before the drug reaches patients.
Does the lower cost of generics imply lower quality?
No. The lower cost is due to the fact that generic manufacturers don't have to pay for the initial research, development, and massive clinical trials that the original brand-name company funded. They only need to prove bioequivalence, which is far less expensive than inventing a new molecule.
Next Steps for Clinical Application
If you are managing a patient with a complex condition and are worried about a switch, start with an A-rated generic. If the patient reports a change in efficacy, don't immediately assume the drug failed. Document the specific lot number and report any suspected issues to the FDA's reporting system to help maintain the integrity of the generic supply chain.
For those dealing with NTI drugs, consider a "slow switch" or more frequent monitoring of blood levels during the first 30 days of the transition. This ensures that individual variability-which exists regardless of whether the drug is brand or generic-is managed safely.


Comments
12 Comments
Rauf Ronald
This is a great breakdown of the bioequivalence standards. I've seen so many providers get tripped up on the difference between A-rated and B-rated generics, and just having a clear guide on the Orange Book is a game changer for clinical practice. It's all about giving patients that peace of mind by explaining the regulatory side of things rather than just telling them it's the same pill!
Daniel Trezub
Yeah, sounds great on paper, but you're totally ignoring the variance in excipients. Like, sure, the active ingredient is there, but who cares if the binder makes it absorb differently in a real-world gut environment vs a sterile lab test? It's all a bit too convenient.
Del Bourne
To add to the point about Narrow Therapeutic Index drugs, I highly recommend that providers implement a mandatory follow-up check within two weeks of switching a patient to a generic. Even with A-rating, individual metabolic responses can vary, and a quick serum level check can prevent a potential crisis before it starts.
Vivek Hattangadi
Totally agree with the approach of using the 80-125% rule to explain things to patients! It turns a scary conversation into a science-based one. I think we can all collaborate more on sharing which specific generic brands have the highest patient satisfaction in our clinics to help each other out. Let's keep pushing for better access through these high-quality generics!
Windy Phillips
One simply cannot ignore the psychological trauma of being forced onto a generic... if the provider even cares enough to explain it... which is doubtful...!!!
Srikanth Makineni
orange book is key. stop overthinking it
Kathleen Painter
I think it's really important to consider that the patients who feel a difference are often the ones who have spent years building a relationship with a specific brand and a specific ritual of taking that medication, and when you change the color or the shape, you're not just changing a chemical but you're disrupting a psychological anchor they've relied on for stability, which is why we should be patient and gentle with them when they express doubt. It's not just about the pharmacokinetics; it's about the human experience of illness and the small things that make a patient feel safe and cared for in a healthcare system that often feels cold and mechanical. If we can just listen to their concerns without dismissing them as a placebo effect, we can transition them to generics more effectively while maintaining that trust. It's a slow process, but it's the only way to truly practice inclusive medicine where the patient feels seen as a whole person and not just a set of clinical outcomes or a line item in a budget. We should really encourage more providers to take that extra five minutes to just sit with the patient and acknowledge that change is hard, regardless of whether the drug is A-rated or not. By bridging that emotional gap, we actually make the clinical transition safer because the patient is more likely to adhere to the new regimen if they feel their anxiety has been validated. It's all about that balance between the hard data and the soft skills of care.
Timothy Burroughs
USA makes the best drugs anyway why are we talking about other countries generic garbage man just stick to american brands and stop complaining about the price it's a small price for quality
Nikhil Bhatia
Too much reading.
Ruth Swansburg
Excellent insights. We must prioritize patient education!
Dhriti Chhabra
It is my humble opinion that the distinction between authorized generics and traditional generics provides a necessary middle ground for those patients who struggle with the transition.
Rupert McKelvie
It is truly heartening to see such clear evidence that affordable medicine doesn't have to mean lower quality. This will help so many people get the care they need.
Write a comment